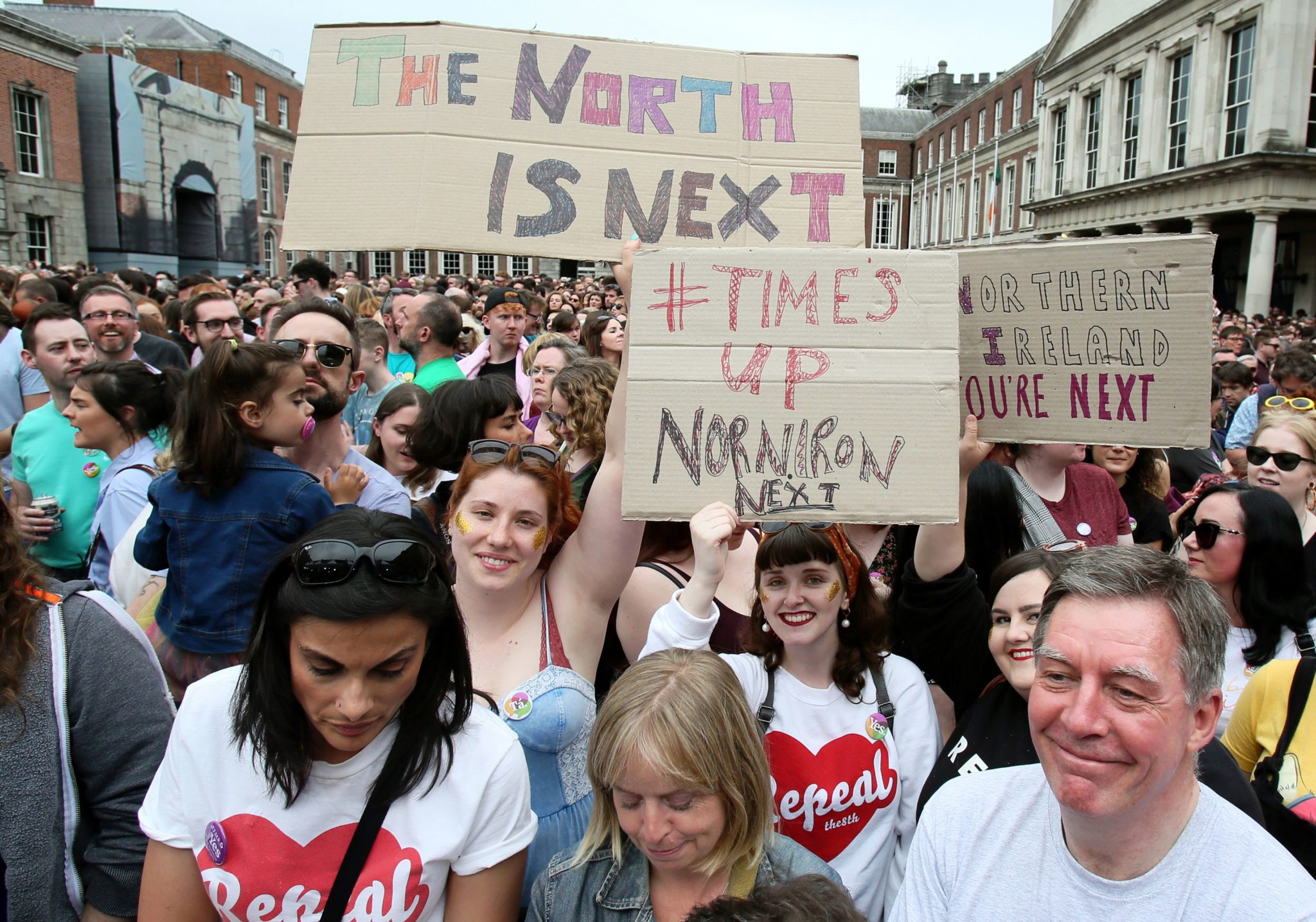Obstacles include sporadic, under-resourced and understaffed services; conscience-based refusals, misinformation as well as pervasive stigma
Introduction of telemedicine – already available across the rest of the UK – would enhance access particularly for those who are marginalised
‘Four years on from decriminalisation of abortion in Northern Ireland, access is a right but not a reality for all who need it’ – Gráinne Teggart
Four years on from decriminalisation, significant barriers to abortion care in Northern Ireland remain, Amnesty International said in a new report published today (07 Dec).
The 159-page report, Legal but not local: Barriers to accessing abortion services in Northern Ireland, lays bare the failures and wide-ranging obstacles facing access to this essential healthcare.
The research, conducted between September 2022 and August 2023 and which tracks barriers to the end of August 2023, is based on desktop research, freedom of information requests and over 60 interviews with women, healthcare providers, healthcare professional bodies, civil society representatives, academics and government representatives concerning access to abortion services in Northern Ireland.
Gráinne Teggart, Amnesty International UK’s Northern Ireland Deputy Director, said:
“Four years on from decriminalisation of abortion in Northern Ireland, access is a right but not a reality for all who need it.
“The report identifies barriers preventing access to this vital and time-sensitive healthcare which must be addressed.
“Abortion care which prioritises a person’s needs and provides impartial advice, is local and is a safe space, should be the minimum anyone can expect.
“Telemedicine must be introduced without further delay. It will particularly benefit those who face other forms of discrimination or barriers in access to healthcare – whether that’s people who live in rural areas, have limited or no access to transport, are in violent or coercive relationships or are concerned about confidentiality.
“We recognise that commissioning is an ongoing process and services are slowly being set up, but the harmful reality of full provision not being available is of significant concern.
“The recommendations in this report chart a way to deliver human rights compliant care and should be actioned immediately.
“Choice must mean choice: in practice and not just on paper. By now, this historic legal reform should be giving people safe access to the full range of abortion services. We must see a faster pace of change.
“Access to quality abortion healthcare is not optional – it’s an essential human right.”
Telemedicine: Legal barriers remain
Since 2020, when Northern Ireland’s current legal framework on abortion came into effect, hundreds of women and girls* have been forced to travel to England or elsewhere for abortion care or opt for online abortion services.
A particularly significant barrier is the lack of self-care interventions for abortion, including telemedicine. Such limitations on self-care are felt most by people facing obstacles and discrimination in access to healthcare more generally – this includes people who live in rural areas, have limited or no access to transport, are in violent or coercive relationships, have certain health conditions, have childcare or other caring responsibilities, have inflexible workplaces and precarious employment and are concerned about confidentiality.
Although the Northern Ireland Department of Health has the power to introduce telemedicine – as England, Scotland and Wales have all done – it has so far failed to do so. When questioned by Amnesty on why this is, they claim that they do not have the authority to make this change. Yet regulations provide approval for abortion medication to be delivered by telemedicine and the Department of Health is authorised to do this under Section 8 of The Abortion (No 2) Regulations 2020, as also recommended by the World Health Organisation.
Conscience-based refusals
A range of people who are not permitted to object to helping a person access abortion services – including administrative staff and an interpreter – have refused to assist people access this healthcare. In addition to this, there are currently no Department of Health guidelines or oversight of this issue.
Misinformation about the permissible scope of conscience-based refusal has been raised as a barrier to establishing and accessing abortion services in almost every interview Amnesty held with healthcare providers and those working to support people to access services.
Many stakeholders expressed concerns about the extent of the practice and the resulting impact on abortion service delivery.
Lack of information, misinformation and stigma allowed to flourish
Public awareness about the abortion law and services remains shockingly low and women face anti-abortion “clinics” eager to mislead and misinform.
Some healthcare providers also lack access to information about the current abortion law and how and where to access abortion services, with concerning repercussions for those seeking abortion services.
In December last year, after the Secretary of State’s instruction to the Department of Health to commission abortion services, information on the abortion law and how to access abortion services was finally made publicly available on NIDirect. However, the information on the website about Northern Ireland’s abortion law is unclear and incomplete.
To date, the Department of Health has not undertaken an awareness-raising campaign to inform the public about the law and how to access available services.
Additionally, the Department of Health has failed to disclose comprehensive annual data on abortion to the public. Publicly accessible disaggregated data is critical to informing policy and improving service provision as well as dismantling the stigma and silence that have long surrounded abortion in the region.
Looking ahead: Urgent intervention needed
It is clear the situation in Northern Ireland needs addressing urgently – without action more people’s rights to essential healthcare will continue to be blocked. The report contains comprehensive recommendations to a range of government departments and public authorities. These can be viewed pages 132-140 of the report. Key recommendations are below.
Amnesty is calling on the Department of Health and the Secretary of State for Northern Ireland to:
- Ensure the full provision of abortion services, including that abortion is available locally across all health trusts and at all gestations, and that patients have a choice of abortion method.
- Ensure that all abortion service provision respects patients’ rights to physical and mental health and autonomy in decision-making, including informed choice.
Amnesty is calling on the Department of Health to:
- Provide and publish written approval for medication abortion to be delivered by telemedicine, as the department is authorised to do under Section 8 of The Abortion Regulations 2020, and as allowed in other parts of the UK.
- Issue evidence-based guidance for registered medical professionals that includes a comprehensive explanation of the circumstances under which abortion is lawful and the lawful scope of conscience-based refusals.
- Exercise oversight over conscience-based refusals to provide abortion treatment.
Ensure that a range of healthcare providers – including nurses and midwives – receive clinical training on abortion service provision, as per WHO recommendations on task sharing on abortion.
Initiate a public information campaign to inform people living in Northern Ireland of the abortion law, existing abortion services, and how to access those services. Ensure this awareness campaign tackles abortion stigma.